By Drew Christensen, MD
Did you know that Hashimoto’s is the most common autoimmune condition in the world?1 Experts predict that if current trends continue, Hashimoto’s or another thyroid disorder will affect 1 in 5 women in their lifetime. (Currently, it affects 1 in 8 women).
This is a sobering statistic, especially because many people don’t even know they have a thyroid disorder, yet they are suffering unnecessarily every day with the symptoms — which they may have been told is a “normal part of aging”.
 Symptoms of thyroid disorders include weight gain, hair loss, low energy, trouble remembering things, brain fog, numbness or tingling of the hands and feet, low libido and more. Find out if you’re at risk here.
Symptoms of thyroid disorders include weight gain, hair loss, low energy, trouble remembering things, brain fog, numbness or tingling of the hands and feet, low libido and more. Find out if you’re at risk here.
These are not “normal signs of aging” — these are warning signs that something is likely amiss with the thyroid. Sadly, when left untreated, thyroid disease can permanently damage the thyroid gland, which can cause problems in every body system and destroy health.
However, when the root causes of Hashimoto’s or any thyroid disorder are addressed, the progression of the disease can be slowed and even reversed. I have seen this happen with many of my patients. I offer free classes in my clinic, Living Health MD, every month on thyroid health. Learn more here.
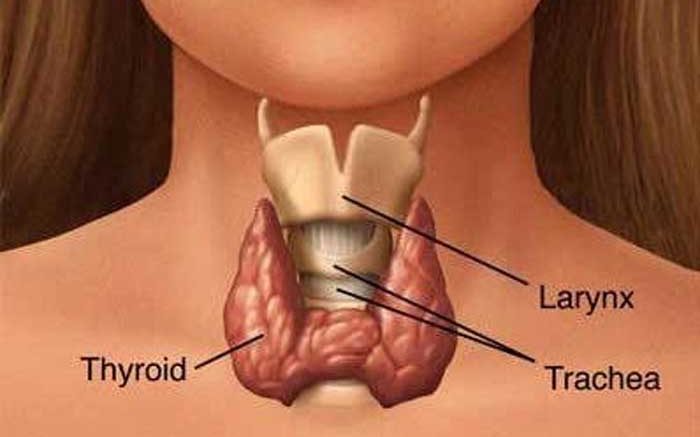
Hashimoto’s thyroiditis is an autoimmune disease where the immune system attacks the thyroid gland as if it were a foreign invader, a virus, bacteria or pathogen.
Left unchecked, the thyroid gland will eventually be damaged so badly it will be unable to produce enough thyroid hormone for the body. This, in turn, leads to all kinds of health problems.
Many people who’ve been diagnosed with hypothyroid disease have been told that they just have a “sluggish” or “under-active” thyroid, that they need to take synthetic thyroid medicine for the rest of their life, and that they are powerless to change their condition.
Another problem is that many patients with thyroid problems never have laboratory tests done to see if their thyroid problem is an autoimmune disease. Those that do have autoimmune thyroid disease, or Hashimoto’s, are often told there is nothing they can do about it.
But there IS something they can do! A lot, in fact! Science is showing us that it’s possible to put some thyroid disorders into remission and eliminate symptoms, reduce thyroid antibodies, and improve thyroid function. With the right interventions, I’ve seen many patients do this, including my own daughter.
Three factors must be present for Hashimoto’s autoimmunity to develop:
* The genetic predisposition
* Triggers that turn on the genes
* Intestinal permeability (leaky gut)
While we can’t change our genes, we can influence the expression of those genes, and the other two factors can most definitely be addressed.
You may have a genetic predisposition for Hashimoto’s disease, but does that mean you’ll get it?
Not necessarily. From the study of epigenetics, we’ve learned that our genes are not our destiny. It is estimated that 90% of chronic disease is not due to our genes but to our environment.2 This is great news because you can control most of your environment – the food you eat, the water you drink, the products you use, and the life you live!

If you avoid the triggers for thyroid disease and eat in a way that prevents intestinal permeability from developing (or change the way you eat to heal it), chances are, you will not get Hashimoto’s disease, or, if you already have it, you can heal and improve your health.
If you have any of the symptoms listed above or suspect you may have a thyroid issue, then please don’t put off taking action to stop the progression of the disease. Your future health is at stake!
Please take this thyroid quiz now and find out what your risk is!
Learn more at our free class, “5 Ways to Improve Thyroid Health and Energy” here.
Living Health MD
1280 S. 20th Ave., Safford, AZ 85546
928-424-4505
Sources:
1 Caturegli P, De Remigis A, Chuang K, Dembele M, Iwama A, Iwama S. Hashimoto’s thyroiditis: celebrating the centennial through the lens of the Johns Hopkins hospital surgical path
2 Journal of Exposure Science and Environmental Epidemiology (2011) 21, 5–9
Sponsored Article